Psoriasis: 10 natural approaches (treatments, dietary supplements ...)
One of the most stigmatising of diseases, psoriasis has a profound physical and psychological impact on anyone who suffers from it. Discover our 10 practical tips to help you cope better with your condition day-to-day.
Psoriasis: what exactly is it?
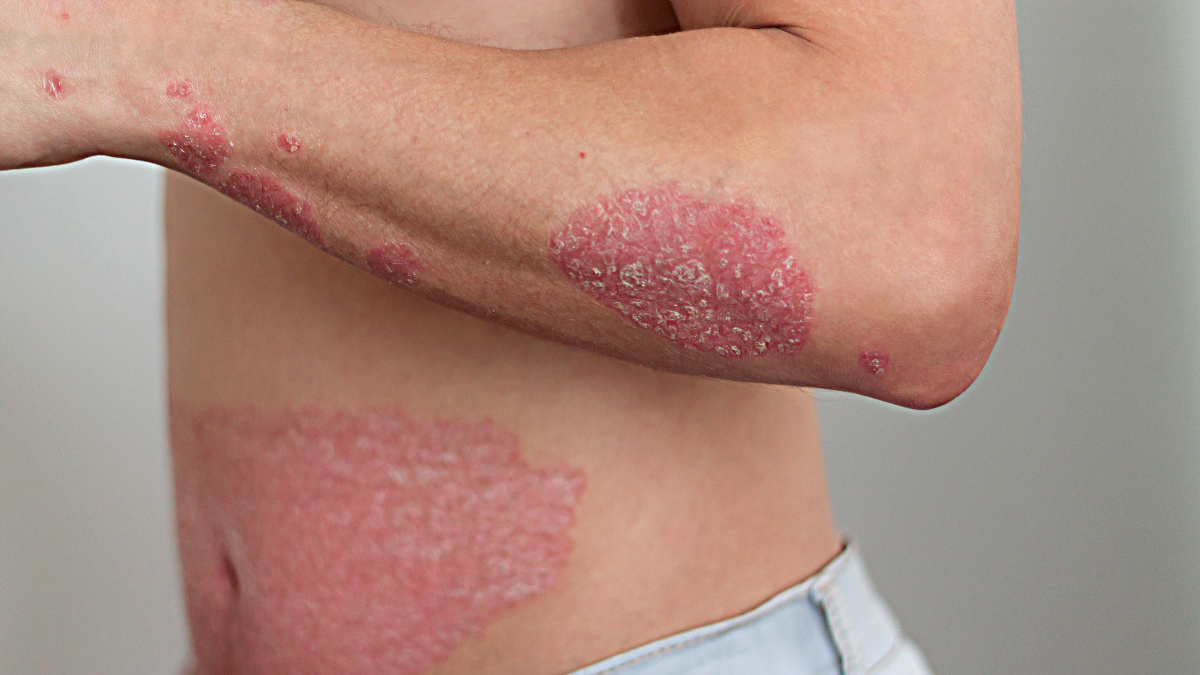
Psoriasis is an inflammatory skin disease of multifactorial origin, characterised by the appearance of flaky, red plaques on various parts of the body (1). Sufferers generally experience flare-ups interspersed with periods of remission.
It’s now known that this chronic disease is caused by immune cells mistakenly attacking skin cells(2). This generates excessive skin inflammation and stimulates the production of keratinocytes (keratin-producing cells). Large numbers of these still-immature keratinocytes accumulate on the skin’s surface, producing a thickening of the stratum corneum (the outermost layer of the epidermis) and scaliness.
In its milder forms, psoriasis primarily affects areas of friction (elbows, knees, forearms, lower back…), the scalp and nails. In severe cases, it can affect the whole body, including the face and mucous membranes – and be complicated by rheumatic or metabolic damage(3).
According to the WHO, around 125 million people globally are affected by psoriasis, with onset peaking between the ages of 20 and 40(4). Though its causes remain poorly understood, there is a strong genetic predisposition (around a third of sufferers have a family history of the disease). Factors such as stress, alcohol consumption, changes in the weather, infections and certain drugs can all trigger flare-ups (5).
As there is currently no cure for psoriasis, the aim is to reduce symptoms in order to improve the quality of life for sufferers. As a first line treatment, vitamin D- or cortisone-based creams can be applied topically. When large areas of the body are affected, immunosuppressive drugs, or UVB light therapy, may be prescribed. For treatment-resistant forms, biotherapy (injections of monoclonal antibodies) offers remission in 75% of cases (6). Whichever the case, it’s always important to follow the advice of your health professional.
In addition, there are some simple everyday steps you can take to help minimise the discomfort of psoriasis and even reduce the frequency of flare-ups.
Keep your skin well-hydrated
Psoriasis very often causes itching(7), but scratching only makes the skin flake even more. To limit these effects, make sure you moisturise your skin well by applying a hydrating cream at least once a day, focusing on scaly patches (8).
Prevent trauma to your scalp
Scalppsoriasis is particularly challenging, as hair shafts make it harder for any treatment to penetrate and adhere (9).
In addition to applying the topical creams prescribed by your doctor, try to avoid inflicting trauma on your scalp as it will maintain or aggravate inflammation: using hair-dryers on too hot a setting, wearing hairbands, headbands, headscarves… Hold your hairdryer at least 20 cm away from your scalp and use a soft brush.
Make sure you get enough vitamin A
While the link between psoriasis and levels of vitamin A is still unclear, a study in 2011 showed that psoriasis patients had lower skin concentrations of carotenoids, a type of vitamin A, than healthy subjects (10). More generally, it’s worth noting that this vitamin is known to play a role in maintaining healthy skin and normal immune system function(11-12).
To correct any deficiency, make sure you eat plenty of yellow-orange fruits and vegetables such as squash, carrots, sweet potatoes and corn. After checking with your doctor, you could also supplement with carotenoids (the product Carottol offers a combination of beta-carotene, lutein, zeaxanthin and astaxanthin in a single capsule) (13).
Avoid perfume (and essential oils)
During a psoriasis flare-up, the skin becomes more permeable to allergens. Dermatologists therefore recommend avoiding perfume and essential oils that may contain it (14).
Aloe vera, the plant for problem skin
Obtained from the leaves of the aloe plant, aloe vera gel has a high mucilage content, giving it emollient and softening properties. It was traditionally used by the ancient Mesopotamian and Egyptian civilisations to fight various skin infections. Since the 1930s, there has been renewed interest from dermatologists and cosmetologists in the topical use of aloe vera (15). Used internally, this plant also helps to maintain healthy immunity due to its content of the polysaccharide acemannan(16).
In the case of psoriasis, where the skin is under severe stress, it’s important to choose a pure, organic aloe vera gel and apply it directly to affected skin (17).
Wash with Aleppo soap
Cosmetics-wise, Aleppo soap is just about as natural as you can get! Produced from olive oil, laurel oil and soda, it has been popular for more than 3000 years for its cleansing and purifying properties.
The fatty acids it contains means it can reduce hardening of skin plaques and skin discomfort without aggravating psoriatic lesions. It can therefore be used for washing without any problem.
Boost your omega-3 intake
There’s now a clearly-established link between fatty acid consumption and inflammation levels. It’s therefore a good idea to increase your omega-3 intake to counterbalance the high levels of omega-6 in modern diets (which in excess are pro-inflammatory) (18-19).
The best sources of omega-3 are oily fish, rapeseed oil, linseeds and hemp seeds. To ensure an optimal intake, you could also take a supplement of these valuable fatty acids (such as the highly-stable product Super Omega 3, which combines EPA and DHA obtained from sustainable fish sources) (20).
Make an oatmeal paste or poultice
Highly-emollient, oatmeal gently eliminates dead cells and soothes redness (21). Simply add 100g of oatmeal to 5 liters of water and bring to the boil. Once cooled, spread the mixture over affected areas and leave to work for 15 minutes before rinsing off.
Bathe in Dead Sea salt
Healing and detoxifying, Dead Sea salt has long been associated with relieving atopic skin. It’s also helpful for the joint stiffness which can accompany severe psoriasis (22-23). Add 3-4 tbsp to your bath water for guaranteed relaxation!
Take Polypodium leucotomos, the fern for beautiful skin
Part of the Polypodiaceae family, the fern Polypodium leucotomos grows deep in the forests of South and Central America. It has long been used by the indigenous people of Honduras for reducing skin discomfort and maintaining beautiful skin.
Containing caffeic and ferulic acids, both powerful phenolic compounds, its role in photoprotection and mode of interaction with the immune defenses are currently the subject of several scientific studies (24-25).
This therapeutic gem from traditional South American medicine is available in supplement form (such as the product Polypodium leucotomos Extract, stabilised with acacia gum and rice flour for a composition that’s 100% natural).
SuperSmart ADVICE
References
- Nair PA, Badri T. Psoriasis. [Updated 2022 Apr 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448194/
- Rendon A, Schäkel K. Psoriasis Pathogenesis and Treatment. Int J Mol Sci. 2019 Mar 23;20(6):1475. doi: 10.3390/ijms20061475. PMID: 30909615; PMCID: PMC6471628.
- Oliveira Mde F, Rocha Bde O, Duarte GV. Psoriasis: classical and emerging comorbidities. An Bras Dermatol. 2015 Jan-Feb;90(1):9-20. doi: 10.1590/abd1806-4841.20153038. PMID: 25672294; PMCID: PMC4323693.
- Bu J, Ding R, Zhou L, Chen X, Shen E. Epidemiology of Psoriasis and Comorbid Diseases: A Narrative Review. Front Immunol. 2022 Jun 10;13:880201. doi: 10.3389/fimmu.2022.880201. PMID: 35757712; PMCID: PMC9226890.
- Kamiya K, Kishimoto M, Sugai J, Komine M, Ohtsuki M. Risk Factors for the Development of Psoriasis. Int J Mol Sci. 2019 Sep 5;20(18):4347. doi: 10.3390/ijms20184347. PMID: 31491865; PMCID: PMC6769762.
- Rendon A, Schäkel K. Psoriasis Pathogenesis and Treatment. Int J Mol Sci. 2019 Mar 23;20(6):1475. doi: 10.3390/ijms20061475. PMID: 30909615; PMCID: PMC6471628.
- Komiya E, Tominaga M, Kamata Y, Suga Y, Takamori K. Molecular and Cellular Mechanisms of Itch in Psoriasis. Int J Mol Sci. 2020 Nov 9;21(21):8406. doi: 10.3390/ijms21218406. PMID: 33182442; PMCID: PMC7664892.
- Kim SD, Huh CH, Seo KI, Suh DH, Youn JI. Evaluation of skin surface hydration in Korean psoriasis patients: a possible factor influencing psoriasis. Clin Exp Dermatol. 2002 Mar;27(2):147-52. doi: 10.1046/j.1365-2230.2002.00975.x. PMID: 11952709.
- Blakely K, Gooderham M. Management of scalp psoriasis: current perspectives. Psoriasis (Auckl). 2016 Mar 29;6:33-40. doi: 10.2147/PTT.S85330. PMID: 29387592; PMCID: PMC5683126.
- Lima XT, Kimball AB. Skin carotenoid levels in adult patients with psoriasis. J Eur Acad Dermatol Venereol. 2011 Aug;25(8):945-9. doi: 10.1111/j.1468-3083.2010.03888.x. Epub 2010 Nov 4. PMID: 21054574.
- VanBuren CA, Everts HB. Vitamin A in Skin and Hair: An Update. Nutrients. 2022 Jul 19;14(14):2952. doi: 10.3390/nu14142952. PMID: 35889909; PMCID: PMC9324272.
- Huang Z, Liu Y, Qi G, Brand D, Zheng SG. Role of Vitamin A in the Immune System. J Clin Med. 2018 Sep 6;7(9):258. doi: 10.3390/jcm7090258. PMID: 30200565; PMCID: PMC6162863.
- Darvin ME, Sterry W, Lademann J, Vergou T. The Role of Carotenoids in Human Skin. 2011 Dec 16;16(12):10491–506. doi: 10.3390/molecules161210491. PMCID: PMC6264659.
- Jacob SE, Butler D, Herro E. Corticosteroid and fragrance allergy exacerbating scalp psoriasis. J Clin Aesthet Dermatol. 2014 Feb;7(2):54-5. PMID: 24578782; PMCID: PMC3935652.
- Syed TA, Ahmad SA, Holt AH, Ahmad SA, Ahmad SH, Afzal M. Management of psoriasis with Aloe vera extract in a hydrophilic cream: a placebo-controlled, double-blind study. Trop Med Int Health. 1996 Aug;1(4):505-9. doi: 10.1046/j.1365-3156.1996.d01-91.x. PMID: 8765459.
- Sierra-García GD, Castro-Ríos R, González-Horta A, Lara-Arias J, Chávez-Montes A. Acemannan, an extracted polysaccharide from Aloe vera: A literature review. Nat Prod Commun. 2014 Aug;9(8):1217-21. PMID: 25233608.
- Guo X, Mei N. Aloe vera: A review of toxicity and adverse clinical effects. J Environ Sci Health C Environ Carcinog Ecotoxicol Rev. 2016 Apr 2;34(2):77-96. doi: 10.1080/10590501.2016.1166826. PMID: 26986231; PMCID: PMC6349368.
- Innes JK, Calder PC. Omega-6 fatty acids and inflammation. Prostaglandins Leukot Essent Fatty Acids. 2018 May;132:41-48. doi: 10.1016/j.plefa.2018.03.004. Epub 2018 Mar 22. PMID: 29610056.
- Mori TA, Beilin LJ. Omega-3 fatty acids and inflammation. Curr Atheroscler Rep. 2004 Nov;6(6):461-7. doi: 10.1007/s11883-004-0087-5. PMID: 15485592.
- Clark CCT, Taghizadeh M, Nahavandi M, Jafarnejad S. Efficacy of ω-3 supplementation in patients with psoriasis: a meta-analysis of randomized controlled trials. Clin Rheumatol. 2019 Apr;38(4):977-988. doi: 10.1007/s10067-019-04456-x. Epub 2019 Feb 18. PMID: 30778861.
- Clark CCT, Taghizadeh M, Nahavandi M, Jafarnejad S. Efficacy of ω-3 supplementation in patients with psoriasis: a meta-analysis of randomized controlled trials. Clin Rheumatol. 2019 Apr;38(4):977-988. doi: 10.1007/s10067-019-04456-x. Epub 2019 Feb 18. PMID: 30778861.
- Katz U, Shoenfeld Y, Zakin V, Sherer Y, Sukenik S. Scientific evidence of the therapeutic effects of dead sea treatments: a systematic review. Semin Arthritis Rheum. 2012 Oct;42(2):186-200. doi: 10.1016/j.semarthrit.2012.02.006. Epub 2012 Apr 12. PMID: 22503590.
- Emmanuel T, Lybæk D, Johansen C, Iversen L. Effect of Dead Sea Climatotherapy on Psoriasis; A Prospective Cohort Study. Front Med (Lausanne). 2020 Mar 18;7:83. doi: 10.3389/fmed.2020.00083. PMID: 32258044; PMCID: PMC7093374.
- Berman B, Ellis C, Elmets C. Polypodium Leucotomos--An Overview of Basic Investigative Findings. J Drugs Dermatol. 2016 Feb;15(2):224-8. PMID: 26885792; PMCID: PMC5189711.
- Choudhry SZ, Bhatia N, Ceilley R, Hougeir F, Lieberman R, Hamzavi I, Lim HW. Role of oral Polypodium leucotomos extract in dermatologic diseases: a review of the literature. J Drugs Dermatol. 2014 Feb;13(2):148-53. PMID: 24509964.
Keywords
2 Hours
Fast reliable service
Fast reliable service Excellent quality products
MONELL
1 Days
Product Delivery
Ease of ordering and product delivery.
CARTER Rhonda
5 Days
Good vegetarian or vegan products free of gelatin, fast shipping.
Good vegetarian or vegan products free of gelatin, fast shipping.
KRASUK Zack
27 Days
Diversity, Delivery, Quality
The product quality, delivery, pricing and diversity of product makes me a satisfied (contented) customer.
JENKINS Rose
28 Days
Good quality
I've ordered supplements from this company three times now. I feel a difference for sure when I take the supplements, their shipping is fast and their quality is good. I'm glad I found them
Monica G
31 Days
Good products
Good products , fast delivery
Jacqueline
32 Days
fast and quick customer service…
fast and quick customer service products are shipped immediately
Michele Dunn
41 Days
Reliable in all ways as a company and…
Reliable in all ways as a company and products available.
DOMINIC
44 Days
Love Supersmart's products!
Their products work!
Diane
45 Days
Excellent experience, as always.
Very fast delivery. Very high quality products Very well made website: easy to navigate, easy to understand and very good and thorough description of each product. Thumbs up!
BUISSON Laurence
54 Days
Dania is Funia
The experience was great because the representative was so personal with me. She was knowledgeable and friendly. I like that she didn't act like a robot and truly was a quality voice behind a quality company. I will continue to purchase from Supersmart!!
Eric Ostovani
58 Days
no time to do your market research
no time to do your market research
David Schwartz
59 Days
Always follow through with!
Always follow through with!
DOMINIC
60 Days
Good product's good service
Good product's good service
PERCY
61 Days
Excellent
Excellent, thank you!
WRIGHT Connie







